Are SIBO and histamine intolerance linked?

If you’ve been dealing with SIBO and suddenly find yourself reacting to foods you used to tolerate, it can feel like your body has completely changed, often overnight. Healthy foods like tomatoes, avocado, spinach or even leftovers (hello batch cooking!) start triggering strange symptoms.
Flushing. Anxiety. Bloating. Headaches. Heart palpitations.
A few hours down the google rabbit hole later and you find you might have ‘histamine intolerance’, so you assume that histamine (or food) is the problem, but when it comes to SIBO and histamine intolerance, that’s rarely the full story.
SIBO and histamine intolerance- it’s not really an intolerance
Let’s clear up one of the biggest myths: histamine intolerance isn’t usually a true intolerance. Your body isn’t inherently unable to handle histamine and histamine is not the bad guy.
What’s happening instead is histamine overload [1]. A helpful way to think about this is the bucket theory. Your body is constantly:
- Producing histamine
- Taking in histamine from food
- Breaking histamine down and clearing it
This is normal in every human. We all require histamine for survival, as it acts as a vital signalling molecule regulating essential bodily functions including immune responses, digestion, and brain function. If everything is balanced, the system works quietly in the background, but when that balance shifts, the bucket starts to fill faster than it can empty.
Once it overflows, symptoms appear, and SIBO is one of the key things that pushes that system out of balance [2].
Why are SIBO and histamine intolerance linked?
To understand the connection, we need to zoom out and look at what SIBO actually is. It’s often described as ‘too much bacteria in the small intestine’, but we now know it’s a state of small intestinal dysbiosis – an imbalance in the small intestinal microbiome. This imbalance changes how the gut functions on many levels.
It affects how you digest food, how your immune system behaves, and how your gut lining maintains its integrity (or not, in the case of leaky gut). These systems are constantly interacting, and histamine sits right in the middle of them. It’s involved in immune signalling, it’s produced and broken down in the gut, and it also acts as a neurotransmitter. So when the gut environment becomes dysregulated, histamine is often one of the first systems to become affected.
This is why histamine symptoms rarely exist in isolation, instead tending to appear alongside broader gut dysfunction – things like bloating, food sensitivity, fatigue, or changes in bowel habits, and it’s also why focusing on histamine alone can feel like you’re missing something.
Histamine is NOT a root cause of SIBO. It’s the environment in which histamine is being produced, processed, and responded to.
Which SIBO bacteria produce histamine?
Microbiome research shows us that histamine levels aren’t just about what you eat, but are also heavily influenced by your gut bacteria. Some bacteria produce histamine, while others help break it down. In a healthy gut, there’s a balance between the two, but in SIBO, that balance is often lost.
Histamine-producing bacteria
Certain bacteria contain enzymes that convert histidine (an amino acid which we consume in food) into histamine. These include Klebsiella, Escherichia coli (E. coli), Morganella morganii and Proteus species [3] [4] [5] [6].
These are commonly associated with SIBO-related dysbiosis and all belong to a group of bacteria called proteobacteria, which are often linked to gut imbalance and inflammation. When these bacteria become more dominant, histamine production increases internally, which means symptoms don’t always correlate well with what you’ve eaten.
Histamine-degrading bacteria
On the other side, some bacteria help regulate histamine levels. Certain strains of Bifidobacterium and Lactobacillus can help break histamine down or support a more balanced gut environment [7] [8]. In a healthy microbiome, these bacteria help to keep histamine levels within a manageable range, but in SIBO, these beneficial species are often reduced, meaning you lose part of your ability to process histamine effectively. This shifts the balance further towards overload.
This is also where the idea of low histamine probiotics comes in. Rather than adding more histamine-producing strains (found in many multi-strain probiotics), the goal is to support the bacteria that help regulate and degrade histamine, gradually rebalancing the system. I love Lactobacillus rhamnosus GG for this, and have found great success with it with clients when used at appropriate doses [8].
It’s not about adding bacteria in isolation, but about restoring that balance between histamine production and breakdown, which is often where the real symptomatic shift happens.
Is histamine intolerance linked to hydrogen, methane or hydrogen sulphide SIBO?
SIBO is often categorised based on the type of gas produced – hydrogen, methane, or hydrogen sulphide. But when looking at SIBO and histamine intolerance, the gas itself isn’t the most important factor. What matters more is the type of bacteria involved and how they affect histamine production, breakdown, and overall gut sensitivity.
Most of the bacteria that produce histamine, including Klebsiella and E. coli, are typically associated with hydrogen-dominant SIBO These bacteria don’t just produce gas – they also increase histamine production, drive inflammation, and make the gut more reactive overall. This is why symptoms like food sensitivities, skin reactions, anxiety and neurological symptoms are more commonly seen in hydrogen-dominant patterns.
Methane SIBO works a little differently. It’s driven by archaea rather than bacteria, and these don’t produce histamine in the same way. Instead, they tend to slow gut movement, which can indirectly worsen the environment by allowing bacteria more time to ferment and interact with the gut lining.
Hydrogen sulphide SIBO sits somewhere slightly different again. Rather than increasing histamine production directly, hydrogen sulphide can irritate the gut lining and reduce DAO enzyme activity, meaning histamine isn’t cleared as effectively. Over time, this lowers your tolerance, so even normal levels can start triggering symptoms.
So while all three patterns can play a role, histamine symptoms are most commonly linked to a more inflammatory, hydrogen-dominant pattern, where histamine production is higher and the overall system is more reactive. I’ve also seen very high histamine levels present in hydrogen sulphide SIBO sufferers which have resolved as we have addressed the SIBO.
How do SIBO and histamine tolerance symptoms present?
SIBO and histamine intolerance symptoms often don’t follow a neat pattern. Symptoms aren’t just digestive and often feel random.
You might get bloating after eating, but also feel anxious for no clear reason. Or notice your skin flushing, your heart racing, or a strange sense of being on edge. For some people it’s more physical – headaches, dizziness , fatigue, or that wired-but-tired feeling. These are often some of the stranger symptoms of SIBO, and histamine can be a big part of what’s driving them.
You might also notice things like:
- Itchy skin, hives, or rosacea-type flare-ups
- Sinus congestion or a blocked/runny nose after eating
- Heart palpitations or feeling slightly shaky
- Nausea or reflux alongside bloating
- Feeling lightheaded, especially after meals
For others it shows up more through the gut – looser stools, urgency, or often quite extreme bloating. The symptoms can change from day to day too – one day it’s digestive, another day it’s anxiety, another day it’s a reaction to a food that was fine the day before. It can feel disconnected, but it isn’t.
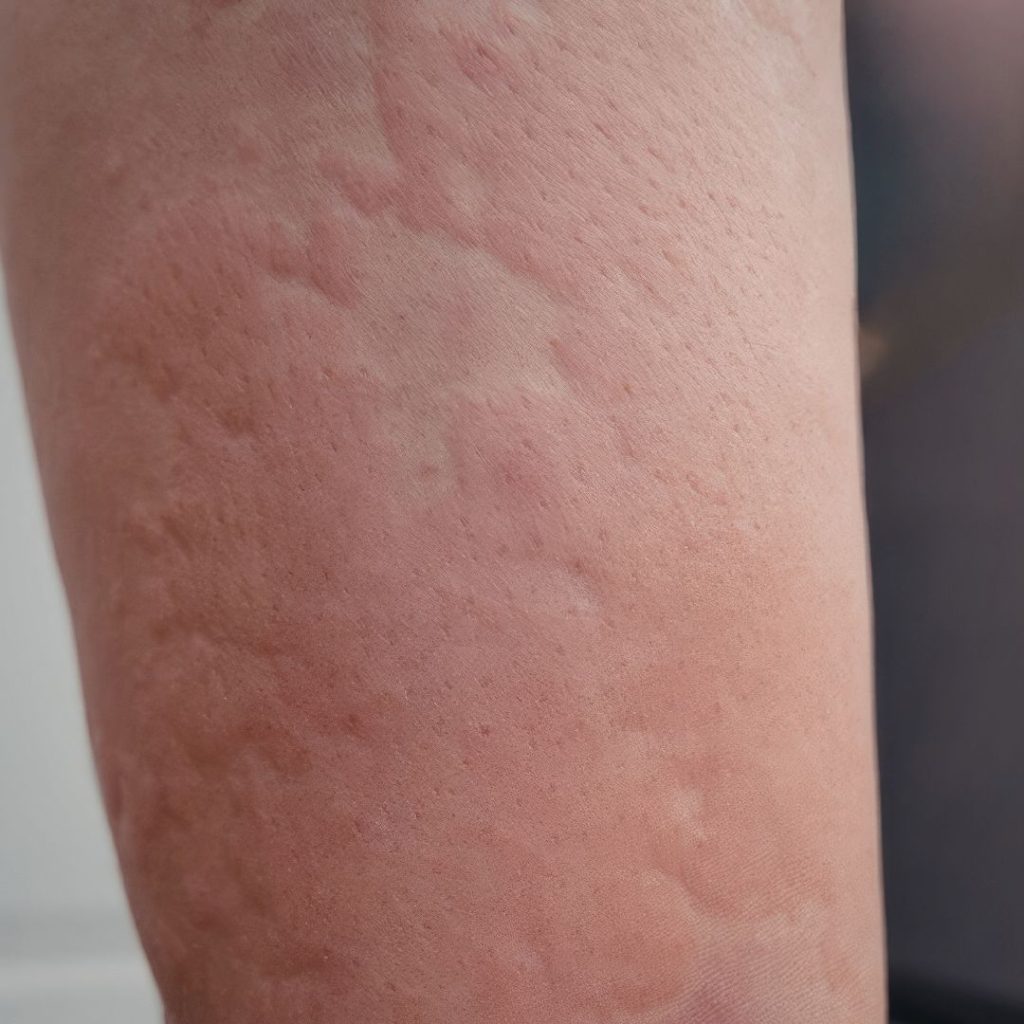
Histamine is involved in all of these systems – the gut, the immune system, the brain – so when it’s out of balance, symptoms can show up in different ways depending on what else is going on in your body at the time. That’s why it’s so easy to end up chasing individual symptoms, rather than seeing the pattern underlying them [1].
Why symptoms don’t follow a clear pattern
One of the most frustrating parts of SIBO and histamine intolerance is how inconsistent everything feels. You might tolerate a food one day, then react to it the next, or feel completely fine in the morning, then suddenly anxious, flushed or bloated later in the day without any obvious trigger.
It can feel random, but there is a pattern underneath it.
Your histamine load is constantly shifting depending on what’s happening in your gut, your nervous system, your hormones, and your environment.
Histamine from food might tip you over, but it’s rarely the only factor. Bacterial production, stress, sleep, and hormonal changes all add to the overall load, while your ability to break histamine down can vary day to day. In SIBO, that balance is disrupted. Histamine production is often higher, breakdown is reduced, and the system becomes more reactive. So the threshold for symptoms becomes much lower.
That’s why something small can suddenly trigger a reaction, and why trying to identify one single problem food often doesn’t work.
Should you do a low histamine diet?
At this point, it’s completely understandable to focus on food. It feels like the one variable in your control, and if eating certain foods triggers symptoms, the logical next step is to remove them. In the (very!) short term, that can help as reducing histamine intake can take some pressure off the system, but it’s important to understand what that’s actually doing.

A low histamine diet doesn’t fix the underlying problem. It simply lowers the amount going into the bucket, and in many cases, food is only a very small contributor compared to what’s being produced internally.
If histamine is being generated by gut bacteria and your ability to break it down is reduced, then food becomes the thing that tips you over, not the thing that’s driving the problem.
That said, a low histamine diet can be useful as a short-term diagnostic tool. If symptoms improve, it can give you a clue that histamine is part of the picture. But it’s not something that should be followed long-term, I wouldn’t keep it in place for more than 4 weeks.
This is why people often find themselves removing more and more foods without fully resolving symptoms: the overall load is still high, so even small inputs continue to trigger reactions. Over time, this can lead to increasing restriction, reduced dietary diversity, and even more imbalance in the gut.
Food may influence symptoms in the short term, but it’s absolutely not where the solution lies.
What actually helps SIBO and histamine intolerance
Put simply, the goal isn’t to eliminate histamine, but to restore your body’s ability to deal with it.
This often looks less like a strict low histamine approach, and more like a broader anti-histamine diet (incorporating antihistamine foods rather than cutting out high histamine foods) and lifestyle – one that supports the gut, reduces inflammation, and lowers the overall histamine load without so much restriction.
That means addressing the underlying drivers:
- Small intestinal dysbiosis
- Gut lining health
- Motility and the migrating motor complex (MMC)
- Nervous system regulation (gut-brain axis)
- Gradual diet expansion rather than restriction
Rather than removing more and more foods, the focus shifts towards supporting a gut environment that is less reactive and better able to process histamine effectively. This is where individual context really matters. The same symptoms can be driven by totally different mechanisms in different people, which is why a one-size-fits-all approach often falls short.
Should I take DAO supplements?
DAO Supplements for histamine intolerance are a common recommendation online, but from both my personal experience and experience with clients, they are extremely expensive and not very effective. There are many other, much more affordable strategies which I would trial in the first instance before DAO supplements.
To sum up:
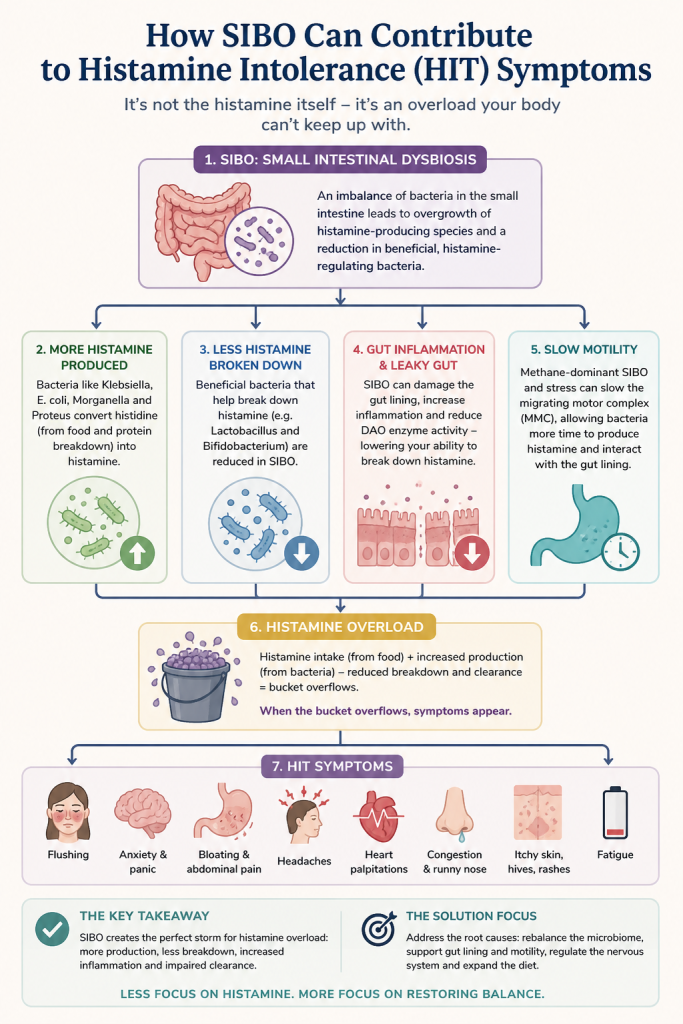
SIBO and histamine intolerance are closely linked, but it’s rarely about histamine alone. It’s an overload problem instead of an intolerance: certain bacteria increase histamine production, beneficial bacteria that help regulate it are reduced, and gut inflammation reduces your ability to break it down, so the bucket fills faster than your body can empty it.
If you’re reacting to more and more foods, it doesn’t mean your body is broken or that you need to keep restricting. It usually means there’s a deeper imbalance driving things, and when you start addressing the bigger picture, the whole system begins to settle.
- https://pmc.ncbi.nlm.nih.gov/articles/PMC11054089/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC9102523/
- https://pubmed.ncbi.nlm.nih.gov/35895832/
- https://pubmed.ncbi.nlm.nih.gov/41515135/
- https://www.sciencedirect.com/science/article/abs/pii/0168160587900328
- https://pubmed.ncbi.nlm.nih.gov/30856743/
- https://www.tandfonline.com/doi/full/10.4161/gmic.25487
- https://pmc.ncbi.nlm.nih.gov/articles/PMC3042653/

My name is Lucy and I’m a Nutritional Therapist specialising in gut health, including SIBO, IBS, functional dyspepsia and histamine-related symptoms. I work with people who feel stuck with ongoing digestive issues despite trying diets, supplements, or standard protocols. My approach focuses on identifying root causes and restoring gut function, alongside supporting the nervous system, rather than relying on restrictive or short-term fixes.
If you’re struggling with persistent gut symptoms and not getting answers, you can book a free gut support call to explore what the right next steps might look like.






